Sjogren's syndrome - oral and dental considerations in HIV/AIDS patients
Developed by the UCSD
School of Medicine,
Copyright 2001, University of California, San Diego with permission.
Copyright 2001, University of California, San Diego with permission.
Thrush
Recognizing the multiple oral manifestations of HIV infection are important clues that may lead you to suspect HIV/AIDS in a first time visiting patient. Often times a previously asymptomatic patient may walk into your office or clinic with the above findings. It then becomes incumbent on you as a physician to identify the underlying immunodeficiency state. In these days, the most important underlying immunocomprised state to identify is HIV/AIDS.
This patient has already been identified as an HIV/AIDS patients who is receiving "the three drug cocktail" therapy. This removable exudate is, of course, thrush. Often times a patient who is dehydrated or has had decreased oral intake may have a "coated" tongue. Clinically, you can differentiate the two by being able to scrape off the Candida with a tongue blade, often times leaving a bloody, painful denudation mark.
As to how to treat this patient there are really two appropriate answers, though one might be better than the other based on the severity of related symptoms. For instance, if this episode of thrush is caught early and has had minimal effects on a patients nutritional intake one could treat with oral mycelex troches. This is preferred since fungal Diflucan resistance can be promoted if one uses this agent repetitively. As such, one would like to save this for a possible future need. However, if the thrush is associated with severe odynophagia, dysphagia and decreased oral intake a short course of Diflucan can help rapidly get the Candida esophagitis under control. Another good candidate for Diflucan would be a patient with repetitive, severe episodes only responsive to Diflucan in the past.
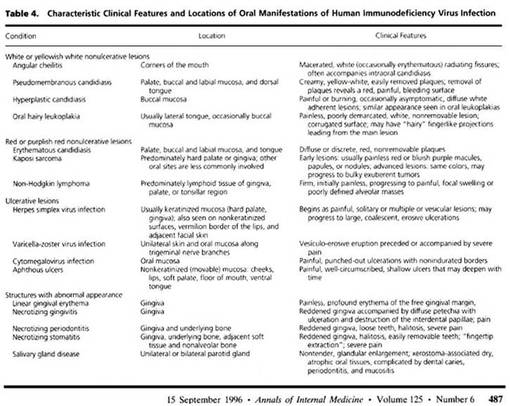
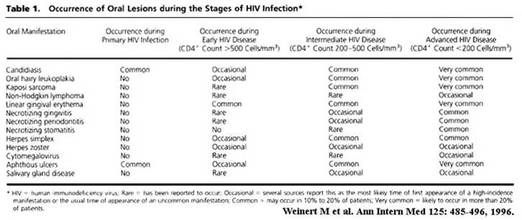
The following tables (1) provide a good listing of the many possible oral lesions identified in the mouth of HIV/AIDS patients:
Recognizing the multiple oral manifestations of HIV infection are important clues that may lead you to suspect HIV/AIDS in a first time visiting patient. Often times a previously asymptomatic patient may walk into your office or clinic with the above findings. It then becomes incumbent on you as a physician to identify the underlying immunodeficiency state. In these days, the most important underlying immunocomprised state to identify is HIV/AIDS.
This patient has already been identified as an HIV/AIDS patients who is receiving "the three drug cocktail" therapy. This removable exudate is, of course, thrush. Often times a patient who is dehydrated or has had decreased oral intake may have a "coated" tongue. Clinically, you can differentiate the two by being able to scrape off the Candida with a tongue blade, often times leaving a bloody, painful denudation mark.
As to how to treat this patient there are really two appropriate answers, though one might be better than the other based on the severity of related symptoms. For instance, if this episode of thrush is caught early and has had minimal effects on a patients nutritional intake one could treat with oral mycelex troches. This is preferred since fungal Diflucan resistance can be promoted if one uses this agent repetitively. As such, one would like to save this for a possible future need. However, if the thrush is associated with severe odynophagia, dysphagia and decreased oral intake a short course of Diflucan can help rapidly get the Candida esophagitis under control. Another good candidate for Diflucan would be a patient with repetitive, severe episodes only responsive to Diflucan in the past.
The following tables (1) provide a good listing of the many possible oral lesions identified in the mouth of HIV/AIDS patients: